Hair loss is incredibly common, but rarely explained properly. This article walks through how healthy hair grows, why it thins, the main types of hair loss, and the biological logic behind modern treatments.
![[headshot]](https://cdn.prod.website-files.com/68207da82e5b8c350c67932f/68c6a7436a552c0fe87a4da7_Screenshot%202024-11-27%20at%2011.38.11.png)
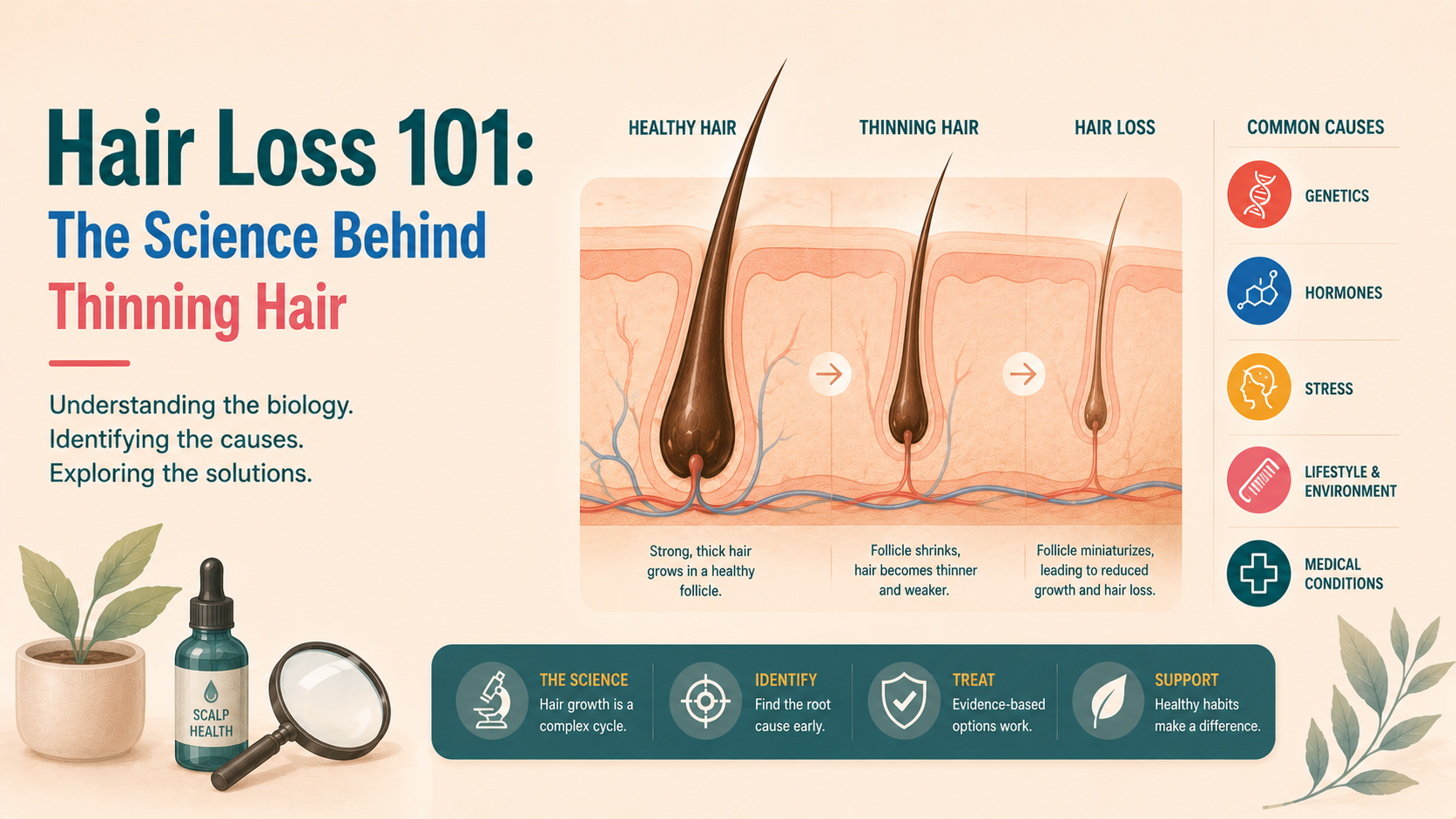
Most hair loss only makes sense once you understand the basics of how hair follicles are built, how they grow in cycles, and how those cycles are disrupted. Hair loss is extremely common, with pattern hair loss being the leading cause, but other conditions like telogen effluvium, alopecia areata and scarring alopecias behave very differently and need different approaches. Modern treatments aren’t random fixes: minoxidil supports the growth phase, anti-androgens reduce harmful hormonal signalling, immune therapies calm inappropriate inflammation, and surgery redistributes resistant follicles. The key takeaway is that accurate diagnosis and early intervention matter because hair loss usually reflects altered follicle biology, not dead follicles, and once scarring occurs, options become limited.
Almost everyone will experience some degree of hair thinning over the course of a lifetime. For some, it is barely noticeable; for others, it becomes one of the defining health concerns of their adult life. Despite this, many people never receive a clear explanation of what is actually happening in their scalp.
Before talking about specific diagnoses or treatments, it helps to understand the fundamentals: how a healthy hair follicle is built, how it cycles, why those cycles go wrong, and how our interventions try to shift the biology back in our favour.
Each hair on your head grows from a tiny, highly specialised organ: the hair follicle.
If you took a cross-section through the scalp, you would see:
The hair shaft itself has three main layers:
Follicles are arranged in units, with one to four terminal hairs often emerging from a single visible pore. Their density, size and orientation all contribute to how “thick” or “thin” hair appears to the eye.
Hair follicles do not constantly produce hair at the same rate. Instead, they cycle through distinct phases:
There can also be a kenogen interval, where the follicle is empty between shedding and the next anagen phase. In health, this is usually brief; in some hair disorders, it becomes prolonged, contributing to visible thinning.
What matters clinically is the balance and quality of these phases. Hair appears full when:
Hair loss is one of the most common concerns seen in dermatology clinics. Broadly:
Scarring alopecia (in which follicles are destroyed and replaced by scar tissue) is less common but clinically significant, requiring early recognition and targeted treatment.
There are many ways to classify hair loss, but a practical starting point is to divide it into non-scarring and scarring forms.
Here, follicles are still structurally present and in principle capable of producing hair, even if they are miniaturised or temporarily inactive.
This is driven by genetically determined sensitivity of certain follicles to dihydrotestosterone (DHT), a metabolite of testosterone.
Key features:
Not everyone with androgenetic alopecia has high circulating androgen levels. Rather, follicles in certain regions have more active 5-α-reductase, more androgen receptors, or a different response to DHT.
This is a reactive shedding, where a larger-than-normal proportion of follicles shift into telogen simultaneously.
Typical triggers:
Mechanistically, a stressor “resets” the hair cycle, causing many anagen follicles to prematurely enter catagen/telogen. Shedding then occurs a few months later. The follicle is not destroyed; given time and removal of the trigger, regrowth is typically achievable.
An autoimmune condition where the body’s own immune system targets the hair follicle, particularly the bulb region in anagen hairs.
Key mechanisms:
Clinically, it presents as smooth, sharply demarcated patches of hair loss that may extend to the entire scalp or body.
In these conditions, the follicular epithelium is destroyed and replaced by fibrous tissue. Once this has occurred, hair cannot regrow from that follicle.
Common examples:
Mechanistically, these disorders involve aberrant immune responses, interface dermatitis, and subsequent scarring. Early diagnosis is crucial, as timely anti-inflammatory treatment can halt progression, but it cannot restore follicles once they are scarred.
Understanding the pathology makes it easier to see why our treatments look the way they do.
Minoxidil is the archetypal example:
Clinically, this translates into longer growth phases, thicker shafts from miniaturised follicles, and more follicles in visible, productive anagen at any one time.
In androgenetic alopecia, the problem is not simply unhealthy hair, but a susceptible follicle in a particular hormonal environment.
5α-reductase inhibitors such as finasteride and dutasteride:
This fits neatly with the observed biology: regions with the highest 5α-reductase activity and androgen receptor expression respond most strongly to systemic DHT reduction.
In alopecia areata and scarring alopecias, inflammation and immune dysfunction become central targets.
Again, the logic flows from pathology: we are not nourishing the hair follicles; rather, we are preventing the immune system from attacking them.
In surgical hair restoration, particularly for androgenetic alopecia, the principle of donor dominance applies:
This is not a cure for the underlying predisposition, but a redistribution of relatively resistant follicles to areas where susceptible follicles have been lost.
For telogen effluvium and some overlapping scenarios, the “treatment” is often to address an underlying imbalance:
The biological rationale is straightforward: if many follicles have been simultaneously induced into telogen, removing the stressor and restoring physiological balance allows them to enter a new, more robust anagen.
This Knowledge Hub will build on these basics, so that when you read about a specific condition or treatment later, the mechanisms underlying it will feel familiar.